Case
The patient was a 49 year-old Caucasian female legal assistant, with a history of mild hypertension, taking hydrochlorthiazide and metoprolol. Chronic leg pain, panniculitis without known primary explanation, and antiphospholipid antibody syndrome (APLS) presenting for a second opinion of lumps in her skin.
The first lump had been noted on her right thigh four years prior to presentation, when the patient noticed darkening of the overlying skin, giving it a bruise-like appearance, with a central nodule. The area itself was non-tender but was associated with lateral leg pain that, according to the patient, failed to respond to physical therapy and multiple cortisone injections. Biopsy of the thigh nodule demonstrated features of a longstanding septal and lobular panniculitis. The nodule was surgically removed and did not recur. After excision of the nodule, the patient’s leg pain decreased, though she felt some residual throbbing, especially at night and with sitting. Approximately six months later she developed two other subcutaneous lumps, on the back and left-lower abdomen. Biopsy of the abdominal lesion was consistent with a lipoma.
Review of systems was unremarkable, as there were no joint pains or swelling of the joints, and no fevers, chills, night sweats, or significant weight change.
Past medical history included hypertension and hypercholesterolemia. The patient had no history of significant thrombotic events and had never been treated with an anticoagulant.
Prior lab investigations, approximately two years prior to presentation in our clinic, revealed an Antinuclear Antibody Test (ANA) that stained positive at dilutions of 1:160 and 1:320, positive anticardiolipin IgM antibody at 93 MPL, and positive Beta-2-glycoprotein 1 IgM antibody at a level greater than 150 MPL. A hematologic panel and coagulation studies were within normal limits. Rheumatologic work-up was also negative for rheumatoid factor, SSA/SSB, and smooth muscle or RNP antibodies. Upon diagnosis of APLS the patient had been placed on 400 mg per day of hydroxychloroquine and 81 mg per day of aspirin.
On exam there was a firm subcutaneous plaque on the left lower back, approximately 3×3 cm, with no overlying skin changes (Figure 1), a firm, mobile nodule, approximately 2×2 cm on the left lower quadrant of the abdomen, and a livedo on the extensor surfaces of the upper arms and legs.
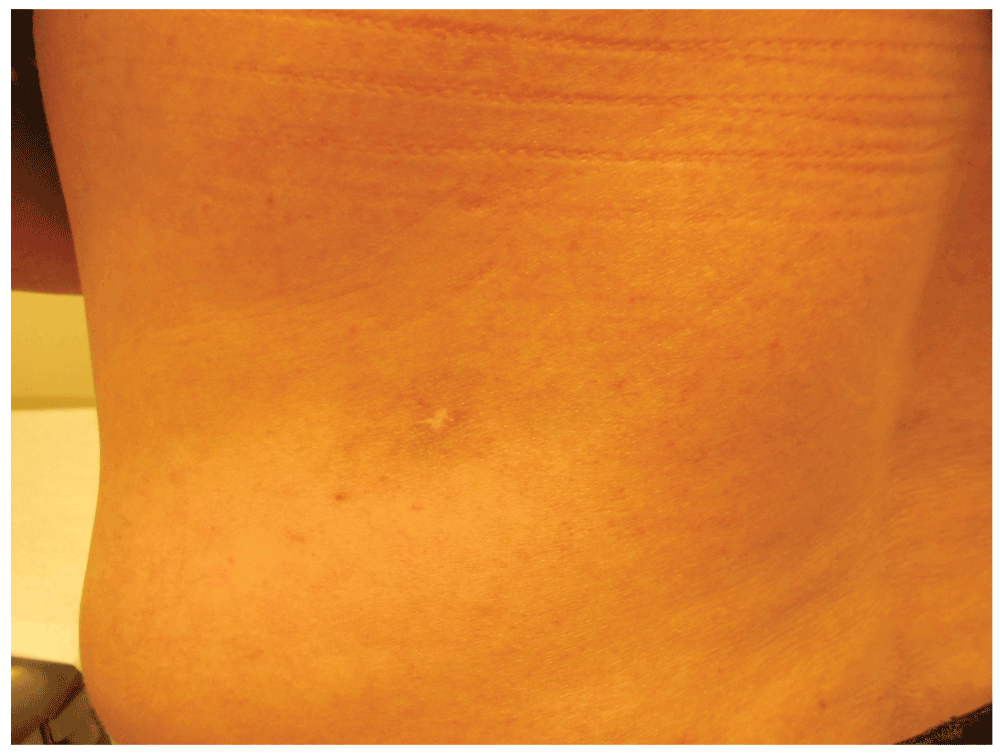
Figure 1. Clinical photograph of RAE lesion.
This photo shows the firm subcutaneous plaque on the patient’s left lower back, approximately 3×3 cm, with no overlying skin changes. On microscopic exam this lesion was found to be RAE.
A biopsy of the patient’s back lesion was reviewed by a dermatopathologist and described as a proliferation of spindled endothelial cells and vessels with concentric wall thickening in the subcutaneous tissue (Figure 2). The spindled cells were highlighted with a CD31 IHC staining (Figure 3), and a Factor XIIIa staining also highlighted many cells within the spindle cell proliferation, confirming their endothelial origin. Additionally, within the dermis there was a perivascular and periadnexal lymphocytic infiltrate. Neither vascular occlusion nor microvascular thrombosis was observed.
Overall, the spindle cell proliferation within the subcutaneous tissue was thought to be suggestive of a reactive angioendotheliomatosis (RAE). In response to this result, the patient’s low dose aspirin and hydroxychloroquine regimen was continued, and she was advised to discontinue oral contraceptive pills (OCPs) given the concern for clotting risk. The patient discontinued OCPs and opted not to have her remaining lesions surgically removed. At six months follow-up, the current lesions have stabilized and no new lesions have developed.
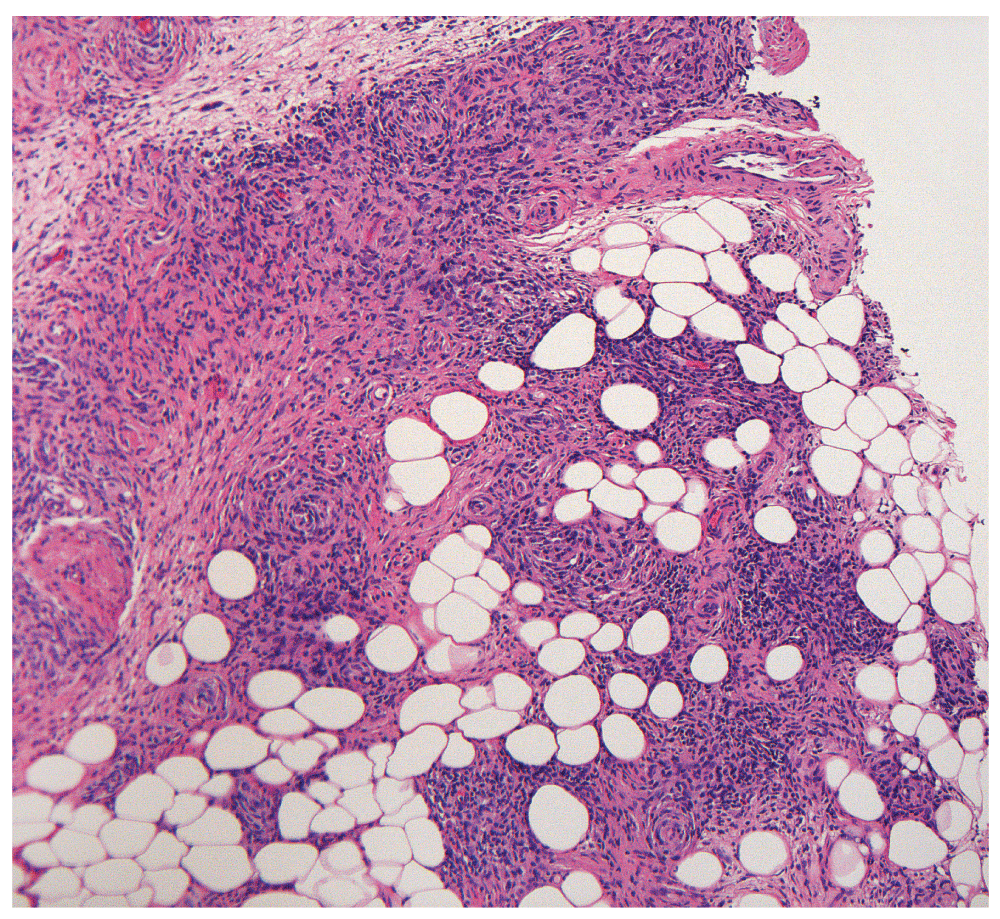
Figure 2. H&E stained section of RAE Lesion at 10×.
An H&E staining of the biopsy section of the patient’s back lesion demonstrating proliferation of spindled endothelial cells and vessels with concentric wall thickening in the subcutaneous tissue. 10× magnification.
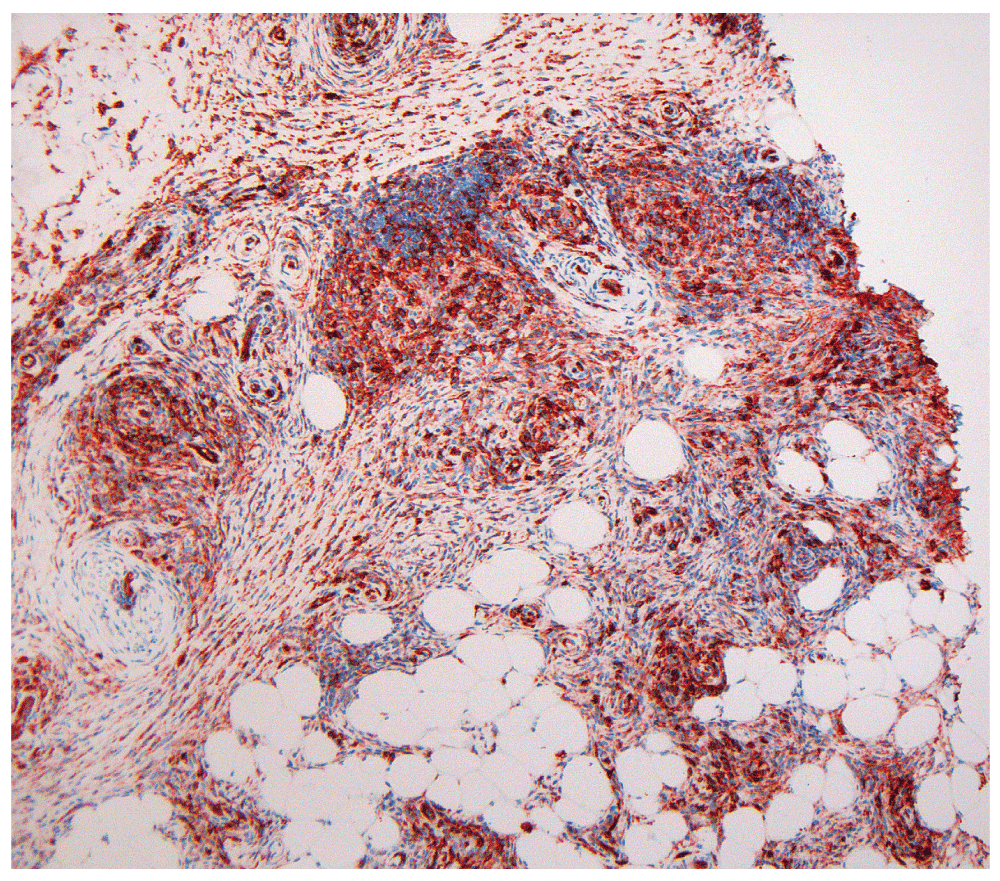
Figure 3. CD31-stained section of RAE Lesion at 10×.
A CD31 immunohistochemical staining of the patient’s back lesion highlighting the spindled cells. 10× magnification.
Discussion
RAE is a benign vascular disorder with a varied clinical presentation that has been associated with a wide range of systemic illnesses. It is characterized histologically by intravascular and extravascular hyperplasia of endothelial cells and pericytes, and this entity only affects the skin1. The intravascular cells are without atypia and have been demonstrated to display reactivity for antibodies to Factor VIII-related antigen, blood group isoantigens A, B, and H, vimentin, and Ulex europaeus I lectin, and negativity for leukocyte common antigen (LCA)2. RAE is very rare, with less than 50 cases reported1. In contrast, malignant angioendotheliomatosis (MAE), a fatal intravascular lymphoma of B-cell origin, displays reactivity for antibodies to LCA, B-Cell antigens, and vimentin in tumor cells2.
Other systemic illnesses that have been associated with RAE include subacute bacterial endocarditis, tuberculosis, lymphoproliferative disorders, liver failure, renal failure, rheumatoid arthritis, cryoglobulinemia, and peripheral vascular atherosclerosis3.
Clinically, the presentation of RAE can vary widely, ranging from erythematous or purpuric papules, macules and plaques to ecchymoses, which may exhibit necrosis or ulceration4. The lesions have been observed to mimic the following diagnoses: Kaposi sarcoma, morphea, pyoderma gangrenosum, calciphylaxis, angiosarcoma, lichen ruber verrucosus, sarcoid, pyogenic granuloma, eruptive disseminated lobular capillary haemangioma, and lupus panniculitus4. The clinical appearance of our patient’s back lesion, an indurated, subcutaneous plaque with no change to the overlying skin, led to a differential of lupus panniculitis versus morphea prior to histological diagnosis.
The pathogenesis of RAE remains unclear, although the fact that it is associated with various disparate disease entities suggests multiple pathways leading to a common reactive pattern3. Additionally, RAE occurs in the context of conditions that may cause occlusion of the vascular lumina. This has led to the suggestion that vascular occlusion by thrombi may cause localized hypoxia and acidosis, followed by hyperplasia of endothelial cells and occasionally pericytes, leading to the observed histopathology5.
In this case, it is likely that the findings of RAE and panniculitis are both associated with the patient’s APLS. Specifically, the pathogenesis of these cutaneous findings has been associated with the presence of anticardiolipin antibodies, which were present in our patient. Localized RAE in the setting of APLS, such as our patient’s back lesion, has been previously described in the literature3, with the first known case reported in 20006 and less than 5 cases reported in total3,5,6. In the context of antiphospholipid syndrome, RAE is likely a result of the procoagulant state induced by the presence of antiphospholipid antibodies. A recent report postulates that the anticardiolipin antibody may be the underlying cause for the thrombophilia leading to the finding of RAE, given that a combination of microthrombosis and reactive endothelial-cell proliferation has been reported in association with anticardiolipin antibodies in the literature5. The patient’s thigh nodule biopsy, which demonstrated panniculitis is also consistent with her diagnosis of APLS. Anticardiolipin antibodies have been associated with septal and lobular panniculitis resembling the features noted in the patient’s biopsy7. Additionally, previous cases have also reported the association of patients with APLS, thigh nodules with leg pain, and elevated anticardiolipin antibody levels7,8. It is unlikely that these cutaneous findings are related to another primary disorder, given the patient’s negative work-up and lack of symptoms indicative for systemic lupus erythematous (SLE), sarcoidosis, fascitis, or scleroderma/morphea, polyarteritis nodosa, or other connective tissue diseases known for producing subcutaneous nodular lesions.
In conclusion, we report the rare case of a woman with both RAE and panniculitis associated with anticardiolipin antibodies in the setting of APLS. This case adds to the literature by describing these rare manifestations of APLS as isolated incidents in a relatively healthy patient.
Consent
Written informed consent for publication of clinical details and clinical images was obtained from the patient.
Author contributions
VW and SS identified this interesting case that warranted reporting. EP prepared the first draft of the manuscript. CS supplied and photographed figures. All authors were involved in the revision of the draft manuscript and have agreed to the final content.
Competing interests
No competing interests were disclosed.
Grant information
This project is supported by the Department of Veterans Affairs Veterans Health Administration, Office of Research and Development, Biomedical Laboratory Research.
The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Faculty Opinions recommendedReferences
- 1.
Rongioletti F, Rebora A:
Cutaneous reactive angiomatoses: patterns and classification of reactive vascular proliferation.
J Am Acad Dermatol.
2003; 49(5): 887–896. PubMed Abstract
| Publisher Full Text
- 2.
Wick MR, Rocamora A:
Reactive and malignant “angioendotheliomatosis”: a discriminant clinicopathological study.
J Cutan Pathol.
1988; 15(5): 260–271. PubMed Abstract
| Publisher Full Text
- 3.
Thai KE, Barrett W, Kossard S:
Reactive angioendotheliomatosis in the setting of antiphospholipid syndrome.
Australas J Dermatol.
2003; 44(2): 151–155. PubMed Abstract
| Publisher Full Text
- 4.
McMenamin ME, Fletcher CD:
Reactive angioendotheliomatosis: a study of 15 cases demonstrating a wide clinicopathologic spectrum.
Am J Surg Pathol.
2002; 26(6): 685–697. PubMed Abstract
- 5.
Kirke S, Angus B, Kesteven PJ, et al.:
Localized reactive angioendotheliomatosis.
Clin Exp Dermatol.
2007; 32(1): 45–47. PubMed Abstract
| Publisher Full Text
- 6.
Creamer D, Black MM, Calonje E:
Reactive angioendotheliomatosis in association with the antiphospholipid syndrome.
J Am Acad Dermatol.
2000; 42(5 Pt 2): 903–906. PubMed Abstract
| Publisher Full Text
- 7.
Hunt RD, Robinson M, Patel R, et al.:
Antiphospholipid-antibody-associated panniculitis.
Dermatol Online J.
2012; 18(12): 18. PubMed Abstract
- 8.
Renfro L, Franks AG Jr, Grodberg M, et al.:
Painful nodules in a young female. Antiphospholipid syndrome.
Arch Dermatol.
1992; 128(6): 847–8. PubMed Abstract
| Publisher Full Text



Comments on this article Comments (0)