Keywords
giant, carotid body, tumor
giant, carotid body, tumor
Giant carotid body tumors are rare. Management of such highly vascular lesions, which completely encase the major carotid artery along with its branches, is even more challenging. We report the management strategy for a similar case, where caudocranial subadventitial dissection completely excised this tumor, one of the largest reported in the literature1,2.
A 22-year-old woman presented to the Neurosurgery clinic in Nobel Teaching Hospital with a history of slow progressive but painless swelling over her left neck, ongoing for the last 6 months. She was also experiencing some difficulty while swallowing. She denied history of trauma, any episodes suggestive of transient ischemic attacks or paroxysmal episodes of severe headache, flushing or chest pain. She did not have major surgery or medical illnesses in the past, or any significant family history.
Local examination revealed a pulsatile swelling on her left neck. There was no audible bruit over the swelling. The patient then underwent a CT angiography, which revealed a well-defined large (> 8 cm) heterogeneous and hyperdense soft tissue lesion; showing intense arterial enhancement at the level of carotid bifurcation (Figure 1). It was causing significant compression and displacement of a long segment of the internal carotid artery (ICA) and external carotid artery (ECA), encasing a broad area of the ICA and ECA ( Shamblin Grade 3) (Figure 2). The lesion was getting vascular supply from both the ICA and ECA branches (Figure 3). These findings were all highly suggestive of a carotid body tumor.
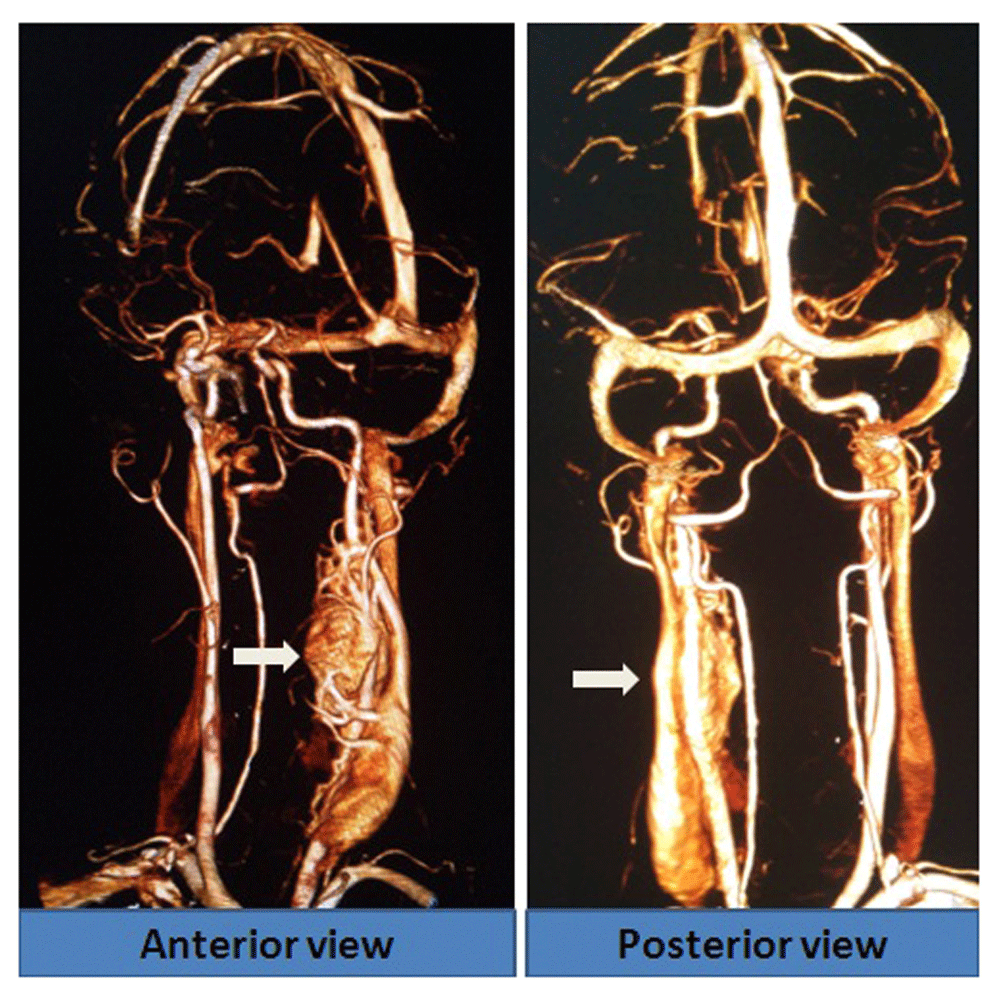
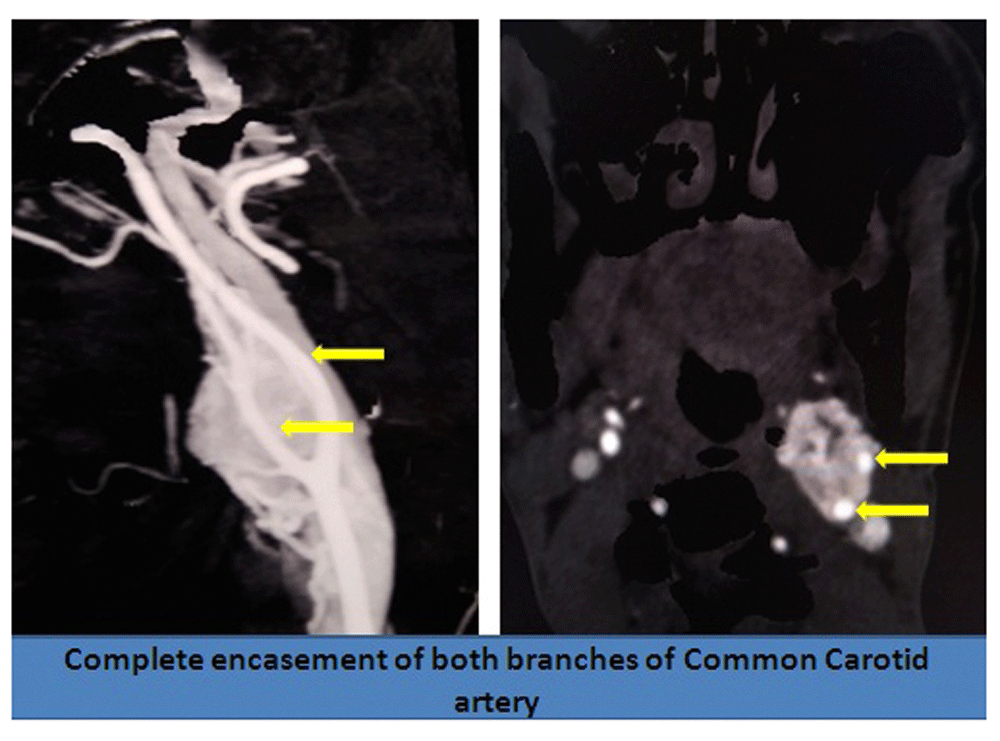
Ultrasound imaging of the abdomen to assess adrenal glands was normal. 24-hour urine vanillylmandelic acid (VMA) and plasma metanephrines were within normal range.
The patient was thoroughly counseled regarding her condition and the need for operative management. The risks associated with the surgery, including intra-operative uncontrolled bleeding, lower cranial nerve palsy, ischemic stroke and even death, were detailed. Anaesthetic precautionary measures were implemented to reduce the risk of hypertensive crisis (during tumor manipulation) and hypotensive episodes (following tumor removal), by administering antihypertensive drugs and fluid support, respectively. After ensuring temporary carotid control with vascular loops, sub-adventitial dissection of the lesion was carried out starting from the common carotid caudally and then progressing cranially towards the bifurcation and its branches (Figure 4). The major vascular supplies were sequentially isolated, ligated and divided. A venous graft from the long saphenous vein was prepared for repair in case of inadvertent tears within the carotid or any of its branches. The internal jugular vein and the vagus nerve within the carotid sheath, and the hypoglossal nerve were all selectively isolated and well preserved. The lesion was completely excised and sent for histopathological analysis. There was only one instance of temporary bradycardia throughout the procedure. Patient made an uneventful recovery with no lower cranial nerve deficits or any vascular insults. The histology from the lesion revealed a characteristic Zellballen pattern, highly suggestive of a Paraganglioma (Figure 5). The patient has been for regular follow-ups in the last 4 months, with complete resolution of her previous symptoms. She has been advised for lifelong periodic visits.
Carotid body tumors, first described by Von Haller in 1743, are of neuro-ectodermal origin3. They are the most common tumors of this origin to occur in the head and neck region4. Since the majority of cases seem to occur in people residing at high altitudes, chronic hypoxemia has been postulated to be a cause for such tumors5. Most patients present with features owing to compression of the lower cranial nerves by the lesion6 In few cases, paroxysmal symptoms resulting from excessive circulating catecholamine may be evident7,8.
Examination should begin by assessing the pulsatility of the tumor. It has a characteristic mobility in the horizontal direction whereas it has restricted mobility in the vertical direction. This aspect is also referred to as the ‘Fontaine sign’9.
Duplex ultrasound study of the carotid vessels is the first line diagnostic imaging modality10. It helps diagnose the lesion, determine its extent and the involvement of the major vessels. It also aids in simultaneous assessment of both the carotid vessels, to rule out bilateral involvement and carotid artery disease, especially in aged patient groups. In high-risk patients with positive family history or in active catecholamine secreting lesions, this type of imaging can help rule out multiple infections by evaluating the adrenal glands. Shamblin et al classified these highly vascular lesions depending on how they are placed in relation to the carotid vessel, which helps plan their management strategy11. Most high-grade lesions require an adjuvant protocol, either in the form of preoperative embolisation or intra-operative temporary or permanent interposition vascular grafts.Needle biopsy is contraindicated due to the risk of haemorrhage, thrombosis or pseudo-aneurysm12. It is also advisable to rule out synchronous neural crest lesions by imaging the tympanic cavity and the adrenal glands, especially in patients with positive family history13. Although rare, active lesions (seen in around 5% of cases) should be ruled out by assessing the plasma catecholamine or the urinary VMA levels14.
The risk of intra-operative and post-operative neurological and the vascular complications increases with the grade of the lesions. The size, vascularity and thereby intra-operative blood loss is minimized with the use of embolisation15. However, there is an inadvertent risk of stroke and increased difficulty in excising the tumor, when it is glued with embolized particles intra-operatively16.
The first successful excision of a carotid body tumor was performed by Albert J Van Der Kogel in 188917. Surgical excision is the management modality of choice, with embolisation and radiotherapy used as adjuncts in a few selected cases10. Cerebral protection from hypotensive insults during vascular clamping or bypass and management of arrhythmias (following vagal nerve stimulation) during tumor manipulation are some of the challenges faced during the intra-operative period18,19. Surgery may be carried out under local, regional or general anesthesia. Local or cervical plexus block offers the advantage of a continuous neurological assessment to rule out cerebral hypo-perfusion20,21. Blood loss can be minimized with meticulous sub-adventitial dissection of the lesion from the vessel walls. Intra-operative vascular control can be achieved by temporary carotid ligation, use of temporary arterial bypass or by use of vascular inter-position graft in cases of inadvertent tear within the vessels22. Hypotensive anesthesia is another valid option to maintain a bloodless field23. A temporary clamp of less than 10 minutes is considered safe13. The IJV, vagus nerve and hypoglossal nerve should always be isolated and well protected throughout the procedure. The higher the grade of the lesion and the need for repair or reconstruction, the higher the risk of stroke24,25.
Huge carotid body paragangliomas continue to cause a high incidence of pre- and postoperative complications17,26, including peri-operative stroke and persistent nerve palsy27.
Cranial nerve palsy is seen in as high as 40% of cases28. The hypoglossal nerve is the most common nerve to be affected in the post-operative period, thereby undue stretching should be avoided. Mortality has been seen in 3% of cases, with tumors greater than 5 cm29. In cases of transmural involvement of the vessel by the tumor, excision of the main vessel along with the tumor is justified. Internal carotid artery ligation with reconstruction requirements as well as permanent cranial nerve deficits have been observed in 23% of cases, all belonging to Shambling grade 3 tumors30.
A characteristic Zellballen pattern in the histology and positive staining with neuron-specific enolase (NSE) for Paraganglioma and S100 for sustentacular cells is definitive in diagnosing the tumor31.
There are no defined pathological criteria to differentiate benign tumors from their malignant counterpart. Distant metastasis and the involvement of the lymph nodes are the only definitive markers to determine its malignant behavior32.
Malignant transformation and local or distant metastasis is estimated to affect around 10% of cases33. Follow-up with doppler and duplex ultrasound of the carotid vessels is currently advocated17.
Lifelong follow-ups are required34. Succinate dehydrogenase (SDH) mutations are commonly seen in young patients, and testing for these may provide us with clues when assessing patients at high risk35.
Large and complicated vascular tumors can be managed with proper planning and execution36. With judicious anesthetic care and meticulous subadventitial dissection, such lesions can be managed even in a rural setup37.
Written informed consent for publication of clinical data and clinical images was obtained from the patient.
| Views | Downloads | |
|---|---|---|
| F1000Research | - | - |
|
PubMed Central
Data from PMC are received and updated monthly.
|
- | - |
Is the background of the case’s history and progression described in sufficient detail?
Yes
Are enough details provided of any physical examination and diagnostic tests, treatment given and outcomes?
Yes
Is sufficient discussion included of the importance of the findings and their relevance to future understanding of disease processes, diagnosis or treatment?
Yes
Is the case presented with sufficient detail to be useful for other practitioners?
Yes
References
1. Hua Q, Xu Z, Jiang Y: Diagnosis and surgical treatment of carotid body tumor: A retrospective analysis of 58 patients.Oncol Lett. 2017; 14 (3): 3628-3632 PubMed Abstract | Publisher Full TextCompeting Interests: No competing interests were disclosed.
Is the background of the case’s history and progression described in sufficient detail?
Yes
Are enough details provided of any physical examination and diagnostic tests, treatment given and outcomes?
Yes
Is sufficient discussion included of the importance of the findings and their relevance to future understanding of disease processes, diagnosis or treatment?
Yes
Is the case presented with sufficient detail to be useful for other practitioners?
Yes
Competing Interests: No competing interests were disclosed.
Is the background of the case’s history and progression described in sufficient detail?
Yes
Are enough details provided of any physical examination and diagnostic tests, treatment given and outcomes?
Yes
Is sufficient discussion included of the importance of the findings and their relevance to future understanding of disease processes, diagnosis or treatment?
Yes
Is the case presented with sufficient detail to be useful for other practitioners?
Yes
Competing Interests: No competing interests were disclosed.
Is the background of the case’s history and progression described in sufficient detail?
Yes
Are enough details provided of any physical examination and diagnostic tests, treatment given and outcomes?
Yes
Is sufficient discussion included of the importance of the findings and their relevance to future understanding of disease processes, diagnosis or treatment?
Yes
Is the case presented with sufficient detail to be useful for other practitioners?
Yes
Competing Interests: No competing interests were disclosed.
Alongside their report, reviewers assign a status to the article:
| Invited Reviewers | ||||
|---|---|---|---|---|
| 1 | 2 | 3 | 4 | |
|
Version 1 04 Oct 17 |
read | read | read | read |
Provide sufficient details of any financial or non-financial competing interests to enable users to assess whether your comments might lead a reasonable person to question your impartiality. Consider the following examples, but note that this is not an exhaustive list:
Sign up for content alerts and receive a weekly or monthly email with all newly published articles
Already registered? Sign in
The email address should be the one you originally registered with F1000.
You registered with F1000 via Google, so we cannot reset your password.
To sign in, please click here.
If you still need help with your Google account password, please click here.
You registered with F1000 via Facebook, so we cannot reset your password.
To sign in, please click here.
If you still need help with your Facebook account password, please click here.
If your email address is registered with us, we will email you instructions to reset your password.
If you think you should have received this email but it has not arrived, please check your spam filters and/or contact for further assistance.
Comments on this article Comments (0)