Keywords
Nonconvulsive seizure; diffuse axonal injury; temporal lobe; excitotoxicity; nonconvulsive status epilepticus
Nonconvulsive seizure; diffuse axonal injury; temporal lobe; excitotoxicity; nonconvulsive status epilepticus
A 13-year-old, medically free student was brought to the King Fahd Hospital of the University (KFHU) after sustaining a motor vehicle accident (MVA) as a car passenger. Due to the side impact, the patient did not sustain any open injuries, and did not eject from the car. No evidence of vomiting, convulsions, nose or ear bleeding was present upon arrival either. However, her consciousness level was fluctuating with intermittent episodes of agitation. On examination, she was drowsy. Her vitals were within normal limits and her Glasgow Coma Scale score was 10/15. Neurological examination did not detect any focal abnormality except a bilateral positive Babinski sign.
Routine blood works and pan body computed tomography scan were normal. Once the patient was admitted to the intensive care unit (ICU), an EEG was requested to rule out non convulsive seizure (NCS) for unexplained altered sensorium. Her first EEG was performed 65 hrs after admission. It detected encephalopathy and electrographic seizures (ESz) arising from the left anterior temporal region (Figure 1), indicating non-convulsive status epilepticus (NCSE). Levetiracetam (LVT) was initiated, and an MRI scan was subsequently performed which revealed multiple hyperintense foci in bilateral frontal and right temporal and occipital lobe, as well as hemorrhage foci on susceptibility weighted image (SWI). These findings were indicative of hemorrhagic axonal diffuse injury type (DAI) type 2. Despite starting LVT, the patient’s consciousness level did not improve; therefore, EEG was repeated after 24 hrs, indicating that NCSE had not been resolved. At this stage, phenytoin was added, after which the patient’s consciousness level improved. The follow-up EEG showed focal epileptic discharges in the form of sharp waves and spikes in the left centrotemporal head region. Patient was discharged on two anti-seizure medications (ASM).
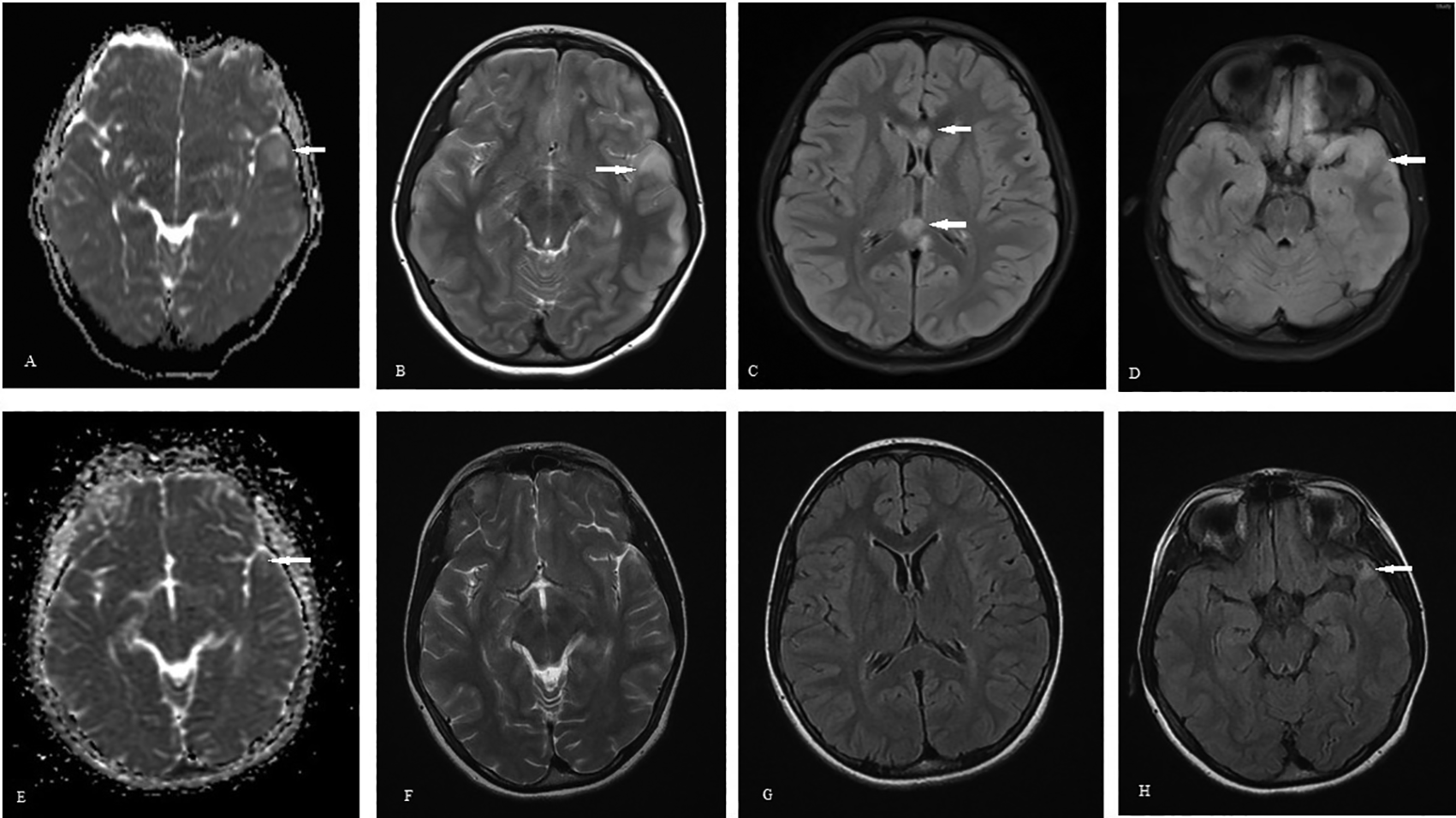
During her follow-up visits, she was symptoms free. Brain MRI and EEG were repeated nine months after the event to determine if ASM should be discontinued. EEG detected focal epileptic discharges in the left temporal head region, and brain MRI showed significant resolution of changes, except an abnormal focal hyperintense lesion in the left temporal area (see Figure 2). Consequently, LVT was continued (the entire timeline is summarized in Figure 3).
One year follow-up, the patient was seizure-free with single ASM and had no symptoms suggestive of cognitive disturbance. She was active in her normal routine life including academics.
TBI is a significant cause of preventable deaths in Saudi Arabia, and 95% are attributed to MVA.1 Seizures (including NCS/NCSE) can occur in 20−30% of patients with severe TBI due to cerebral metabolic distress and hippocampal atrophy, which contribute to higher mortality rates.2 However, in clinical practice, NCS following TBI may remain undiagnosed due to the lack of overt clinical manifestation and adversely affect outcomes due to the delay in treatment.3 Occurrence of early NCS can have subsequent neurologic sequelae due to excitotoxic neuronal injury aggravating the injury caused by TBI.4 Therefore, it is mandatory to diagnose NCSE in a timely manner to prevent significant neurological sequelae by performing EEG in TBI victims with altered sensorium. The benefits of this protocol are supported by the findings yielded by a study involving continuous EEG monitoring in 16 patients with severe TBI, allowing NCS to be detected in three cases.5 Similarly, seizures were detected using EEG in 20% of examined patients, more than 50% of whom experienced NCS.6
Our patient had TBI of moderate severity7 and prolonged NCSE which lasted for five days. Brain MRI showed changes related to prolonged NCS, along with DAI. The follow-up EEG detected focal ED in the left temporal region and MRI showed a small localized hyperintense lesion in the left temporal lobe which could be either a sequela of TBI or NCSE. However, the left temporal cortical edema, which could be the result of prolonged NCS, was completely resolved. The relationship between prolonged NCS and structural changes to the brain, particularly the temporal lobe, has been reported previously.2,8 Vespa et al. examined cEEG findings of 140 patients with moderate to severe TBI, and detected acute post-traumatic NCS in 23% of the cohort. Moreover, in a selected group of patients, this finding was significantly associated with long-term hippocampal atrophy.2 In addition, according to one case report, a patient with schizophrenia and NCSE having increased hippocampal volume in an acute setting was later found to have hippocampal atrophy.8 Although NCSE is not uncommon following TBI, its association with anatomical changes leading to hippocampal atrophy in the long term is debatable, given that significant neuronal damage due to diffuse injury itself can be a cause. Thus, further research is required to better understand these phenomena.9 Jorge et al., studied 37 patients with closed head injury and concluded that hippocampal volumes were significantly lower in patients with moderate to severe head injury than in patients with mild TBI.10
In our patient, follow-up brain MRI showed a significant resolution of findings detected in the initial scan; however, a small abnormal hyperintense signal was persistent in the left anterior temporal region. As volumetric MRI is not available in our healthcare facility, we were unable to assess the volume loss. Still, we posit that—in addition to TBI—prolong NCSE in our patient could be a contributing factor for this finding on follow-up MRI. Although our patient did not have any clinical seizures, follow-up EEG and MRI performed nine months after the initial incident were suggestive of temporal lobe pathology with a heightened risk of temporal lobe-onset seizure. Accordingly, her ASM could not be discontinued. In reporting on this case, our aim is to highlight the importance of close EEG monitoring in patients with TBI in whom consciousness is altered. In this particular case, brain MRI was instrumental for detecting changes not only in DAI but possibly NCS as well.
This case highlights our limitation of immediate EEG recording in patients with TBI upon arrival. The strength is the identification of uncommon electrographic patterns suggesting NCS during routine EEG recording guiding proper management.
This case illustrates the possible association of prolonged NCSE following TBI with temporal lobe structural changes. It further emphasizes the need for immediate EEG monitoring in patients with TBI that present with altered sensorium. All institutes dealing with trauma cases should thus have the resources needed for emergency EEG monitoring to avoid neurological sequelae of NCS, which may otherwise remain undiagnosed.
We confirm that we have obtained permission from the patients’ father to use images and data included in this article.
| Views | Downloads | |
|---|---|---|
| F1000Research | - | - |
|
PubMed Central
Data from PMC are received and updated monthly.
|
- | - |
Is the background of the case’s history and progression described in sufficient detail?
Yes
Are enough details provided of any physical examination and diagnostic tests, treatment given and outcomes?
Partly
Is sufficient discussion included of the importance of the findings and their relevance to future understanding of disease processes, diagnosis or treatment?
Partly
Is the case presented with sufficient detail to be useful for other practitioners?
Partly
References
1. Cartagena AM, Young GB, Lee DH, Mirsattari SM: Reversible and irreversible cranial MRI findings associated with status epilepticus.Epilepsy Behav. 2014; 33: 24-30 PubMed Abstract | Publisher Full TextCompeting Interests: No competing interests were disclosed.
Reviewer Expertise: Electroencephalography, neuroimaging, epilepsy, status epilepticus
Is the background of the case’s history and progression described in sufficient detail?
Yes
Are enough details provided of any physical examination and diagnostic tests, treatment given and outcomes?
Partly
Is sufficient discussion included of the importance of the findings and their relevance to future understanding of disease processes, diagnosis or treatment?
Yes
Is the case presented with sufficient detail to be useful for other practitioners?
Yes
Competing Interests: No competing interests were disclosed.
Reviewer Expertise: Epilepsy, Stroke
Alongside their report, reviewers assign a status to the article:
| Invited Reviewers | ||
|---|---|---|
| 1 | 2 | |
|
Version 2 (revision) 24 Jan 24 |
read | read |
|
Version 1 14 Sep 23 |
read | read |
Provide sufficient details of any financial or non-financial competing interests to enable users to assess whether your comments might lead a reasonable person to question your impartiality. Consider the following examples, but note that this is not an exhaustive list:
Sign up for content alerts and receive a weekly or monthly email with all newly published articles
Already registered? Sign in
The email address should be the one you originally registered with F1000.
You registered with F1000 via Google, so we cannot reset your password.
To sign in, please click here.
If you still need help with your Google account password, please click here.
You registered with F1000 via Facebook, so we cannot reset your password.
To sign in, please click here.
If you still need help with your Facebook account password, please click here.
If your email address is registered with us, we will email you instructions to reset your password.
If you think you should have received this email but it has not arrived, please check your spam filters and/or contact for further assistance.
Comments on this article Comments (0)